For 4-year-old Bryleigh, cancer treatment doesn’t come with a whole lot of choices. She has to do chemotherapy, she has to go through scary procedures like spinal taps and lumbar punctures, she has to stay isolated from her friends when her immune system isn’t strong enough to fight basic illnesses. She has to miss out on a lot of the fun things a vibrant 4-year-old like her should get to experience.
“So much that comes with cancer isn’t her choice,” says Victoria, Bryleigh’s mom. “So I try to give her as much choice as I can in other ways — like we have to do this port access, but how do you want it done? What do you want on your sticker afterward? If we have four medicines we have to take, I’ll ask her which one she wants to take first. I try to give her as much control as I can without taking away from what needs to be done.”
This is just one of the strategies Victoria learned after becoming a cancer parent in April 2024.
Worst-Case Scenario
The first sign that something wasn’t right wasn’t exactly glaring — Bryleigh had a rash, something that looked a little like bruising or broken blood vessels. She’d just gotten back from spending time at her dad’s house, so Victoria reached out to him to ask if anything had happened. She was playing like crazy, he said, but nothing out of the norm. Victoria just had a feeling something was off, so she sent a picture of the rash to the director of nursing at the nursing facility where she works. The director told her to get Bryleigh seen right away.
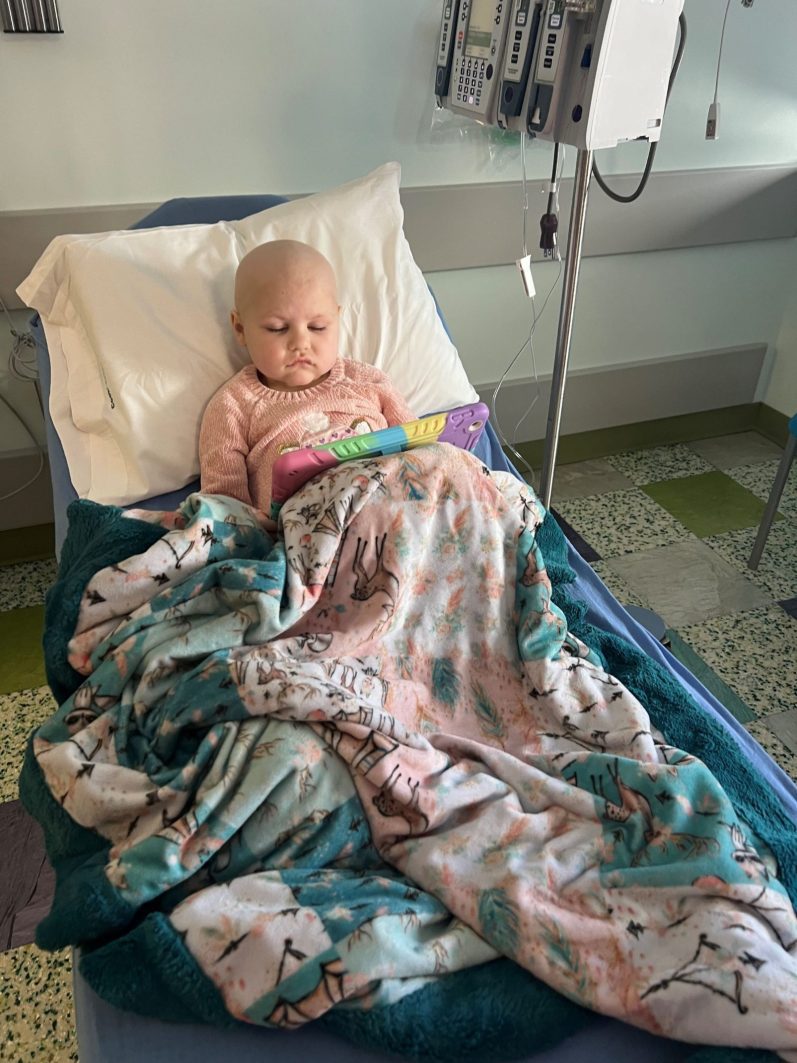
After testing at their local urgent care, Victoria and Bryleigh were sent to the emergency room. Victoria’s job as a social worker in a nursing home means she’s worked closely with those in the medical field. She knows what it looks like when someone is avoiding giving a patient bad news. She knew it was a bad sign that they were fast-tracked through the emergency room, and she had a sense that there was something the doctors weren’t telling her yet.
“I remember asking them, ‘What is the worst-case scenario here? What is the worst thing you think it could be?’” Victoria said. The answer: leukemia. Just a few hours later, bloodwork confirmed the diagnosis — B-cell acute lymphoblastic leukemia — and Victoria’s world turned upside down.
A Steep Learning Curve
From day one, Victoria says it was like having another full-time job — she was suddenly responsible for learning everything she could about childhood leukemia to support the care team’s treatment path for Bryleigh. Long after her little girl had fallen asleep, Victoria would stay up looking things up online, wading through a sea of hard-to-interpret studies and data about ALL.
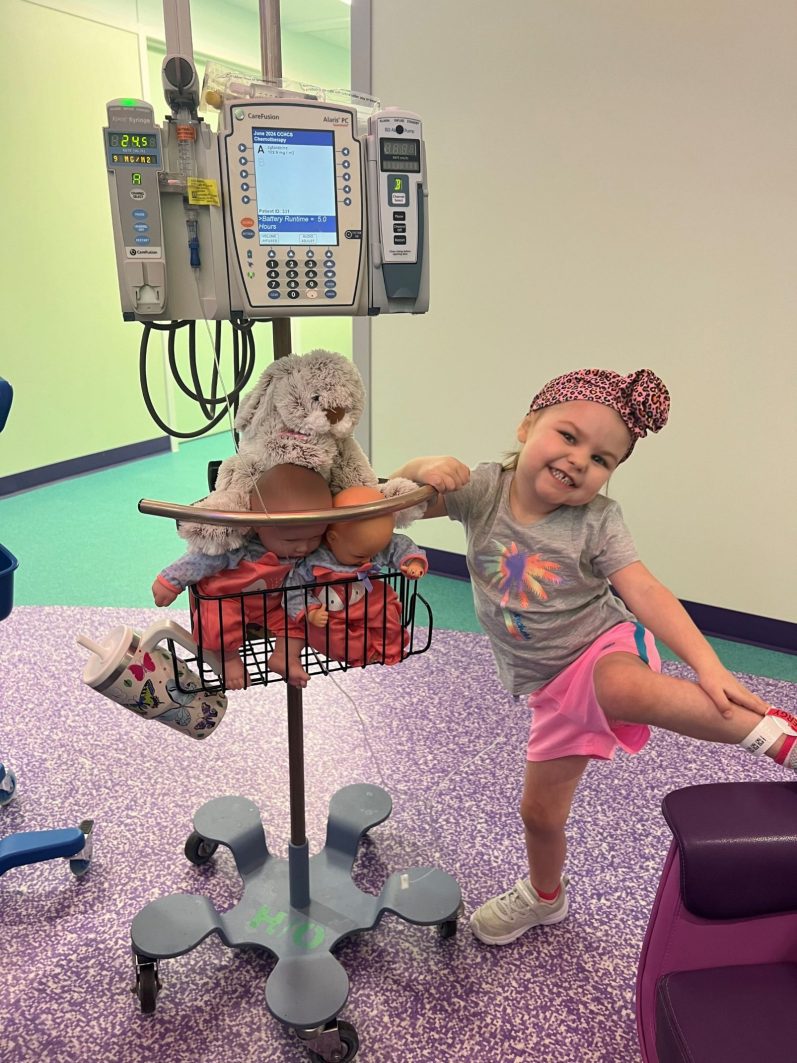
She and Bryleigh’s care team initially decided to enroll her in a clinical trial, which would mean Bryleigh undergoes the typical ALL treatment plus a new immunotherapy drug, blinatumomab, which researchers hope could minimize side effects of treatment and make it less likely for a child’s leukemia to come back. At the end of the induction and consolidation phases of treatment, Bryleigh’s cancer hadn’t gone into remission, which is what they’d been hoping for.
Victoria and Bryleigh’s care team decided to remove her from the clinical trial and move forward with the high-risk standard treatment. Once she achieved remission, she was able to receive Blina again per the clinical trial’s protocol. Through this experience, Victoria has learned how essential childhood cancer research is for kids like Bryleigh, and she’s glad they’ve been able to play a part in furthering research.
“Even though Bryleigh wasn’t able to complete the trial, we’re glad we participated, because now Blina is now a part of frontline treatment for ALL,” Victoria said. “If Bryleigh’s journey can help anyone, then that is her reason to have cancer.”
Victoria also had to figure out how to translate everything she was learning into language a 4-year-old could understand. Victoria knows how to talk to older patients and their families about cancer, but explaining it to a child has been a different experience.
“She knows that her blood is sick and that the treatments we do are to make the sickness go away,” Victoria said. She says she’s been proud to watch her daughter soak up medical terms throughout her cancer experience, but that it’s heartbreaking to hear her ask questions like, “When I get better, can we go to the park? When can I go to school? When I’m better, can we go out to eat?”
“When her counts are down, it’s important that Bryleigh doesn’t get sick, so we don’t go to family members’ houses or any of the places she asks to go,” Victoria said. “So much has been taken from her. Life right now is pretty much home and doctor’s appointments.”

Victoria has become an expert at employing strategies to distract Bryleigh or soothe her through painful or scary moments. During treatment, Bryleigh developed a love for worship music, and Victoria decided to play the song “Jesus Loves Me” during a puncture that had Bryleigh hysterical with fear.
“I just watched her relax from head to toe,” Victoria said. “Now, ‘Jesus Loves Me’ is her go-to song for port access and back pokes. I’m really proud of how her faith has grown to become something astronomical and beautiful through all of this. She sings and she prays — clinging to faith has been a big part of this for both of us.”
Bryleigh still has a long treatment road ahead — the standard treatment for ALL usually lasts between two and three years. Victoria says she wants more people to know that childhood leukemia treatment is a marathon, and that support systems should keep checking in throughout that time to see how the child and family’s needs have changed.
“We all face this crazy world, and we can’t do it alone,” Victoria said. “I feel so blessed by our family and community and everything they’ve given us, and I want to give that feeling to other people. Nobody should have to feel like they’re doing this alone.”
Sharing Hard-Fought Wisdom
Since Bryleigh’s diagnosis, Victoria says she realized how little guidance there is for cancer parents. She’d have given anything for a map that showed a way through this experience. So she’s started creating one — sharing tips with other cancer parents whenever she can. Below are some of the cancer-parent wisdom she’s gathered during Bryleigh’s first year of treatment that she hopes other parents can learn from.
- How do you answer questions like, “How is Bryleigh doing?”
I’m honest and I say things like, “She’s doing well under the circumstances.” Or I tell them that she’s happy that we are at home, but she could still get sick really easily so we have to stay isolated. I don’t sugarcoat cancer treatment — I don’t feel like the hard parts are talked about enough. People try to make it all smiley pictures, but that’s not how it is, so I try to be honest when people ask.
- Where should cancer parents turn for support?
We have so much support from friends and family, both locally and from far away, but getting to know other cancer moms has been essential. On the first day of Bryleigh’s treatment, another mom whose child has AML immediately embraced me and encouraged me to connect with other moms. Any time I meet a new cancer mom, I try to introduce myself and make a connection. I tell them, this is going to be hard, but you can do it. I encourage them to lean on their faith if they have one, and not to be afraid to ask for support. You really need that cancer-mom community, because we’re the ones who get it.
- What practical advice would you give to other parents in your situation?
It’s important to include yourself in the team of your child’s doctors. You don’t have to just follow blindly. Bryleigh has a great care team, and I’ve been able to advocate for certain things because they aren’t with her every moment, they don’t see what I see. You know your child best, and you are a vital part of their care team.




